Residency Accreditation Toolkit: ACGME Milestones and Competency-Based Resident Evaluation
Under the ACGME accreditation system, all residents are evaluated using a competency-based assessment model. This model evaluates residents under six domains of clinical competence. Learn about them and more.
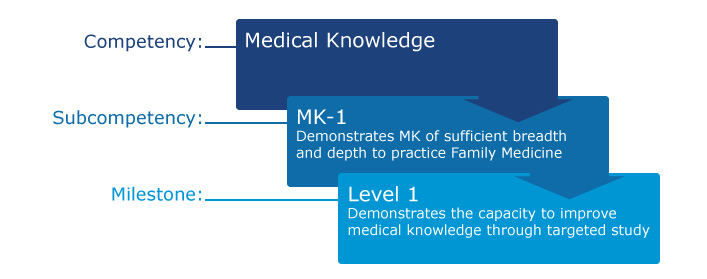
The ACGME accreditation system's competency-based assessment model evaluates residents under six domains of clinical competence: patient care, medical knowledge, systems-based practice, interpersonal and communications skills, and practice-based learning and improvement. These general competencies apply to all specialties.The sub-competencies and milestones, which further divide the general clinical competencies into meaningful components, provide key observable behaviors and are specialty-specific.
ACGME Milestones Background and Design
Residency training requirements have traditionally been based on required amounts of time and volume of experience to certify residents for independent practice. In 2002, the ACGME made a major paradigm shift to focus on observation of competency performing specific required activities of practice to graduate residents. They identified 6 domains of clinic competence common to all specialties that residents would be evaluated for:
- Patient care
- Medical knowledge
- Systems-based practice
- Practice-based learning and improvement
- Interpersonal and communications skills
Within these six competencies each specialty then identified specific sub-competencies required for practice in that specialty. An updated version of the Milestones, Milestones 2.0, went into effect July 2020. The sub-competencies were modified based on user feedback and now provide a more logical progression of skill levels across resident development than in version 1.
Levels of Performance
For each sub-competency in family medicine, specific observable behaviors are listed over 5 levels of performance. Assessing a resident on a sub-competency means looking for those behaviors; when they occur consistently the resident has achieved that level of performance for the sub-competency. The levels are intended to represent:
- Level 1: A resident who has had some education in Family Medicine (R1 entry level).
- Level 2: The resident is advancing and demonstrating additional milestones (R2 level).
- Level 3: The resident consistently demonstrates the majority of milestones targeted for residency (R3 level).
- Level 4: Substantially demonstrates the milestones targeted for residency. This level is designed as the graduation target.
- Level 5: “Aspirational” goals of an experienced family physician. Few residents reach this level.
Residents can be ranked at 0.5 levels also, when they demonstrate some but not all behaviors for the next level up.
Current Milestones Use
Each program is required to report Milestones levels for each resident in the ADS semi-annually as generated by the program’s CCC. This data is informational only, since the Milestones Project is a work in progress and the ACGME is collecting data on current residents to refine and improve the Milestones. The latest version of the Milestones, 2.0, became effective July 2020. The Milestones performance level 4 is intended to be the level for a graduating resident ready for independent practice, but the ACGME specifies that it is not necessarily intended to be a graduation requirement. Program directors are still charged with determining when a resident is ready for graduation.
Should Programs Create Milestone-Based Evaluations?
The ACGME specifically notes that Milestones are not intended to be used as direct observation evaluation tools.Creating Milestone-based evaluations does offer the advantage of providing multiple data points from different observers for the Milestones. However, the ACGME notes that using Milestones-based evaluations only is inadequate to evaluate residents in all areas and programs should consider what additional evaluations are needed. Also, the CCC must still make a summary determination of Milestones levels for each resident semi-annually based on review of all performance data.For programs that use non-Milestones-based evaluations there are 2 basic approaches:
- Have the CCC review the evaluations and determine Milestones levels for the residents, or
- Map their current evaluations to the Milestones, so that each item on an evaluation is given a corresponding sub-competency performance level. This can be an arduous process but does offer the advantage of generating Milestones data that may better guide the CCC’s determination.
Core Outcomes of Family Medicine Education
In 2023, The ACGME Family Medicine Review Committee (FM-RC) and the American Board of Family Medicine established the "core outcomes" of family medicine residency education. The core outcomes represent observable behaviors that can be improved with deliberate practice.Beginning in June 2024, the American Board of Family Medicine will require program directors to attest "both that each resident has finished their residency and is competent in all the core outcomes, "with an additional focus on robust continuity of care, the care of children and more specific aspects of the care of pregnant women." The attestation requirement will be rolled out over 3 years, with the following schedule.2 Programs do not report to the ACGME on the core outcomes.
